|
What are Fungal Eye Infections?
Are your eye(s) burning? Are they red, tearing, possibly painful, sensitive to light and/or releasing a white or yellow discharge? You may have an Eye Infection. Eye Infections can give a wide gamut of presentations from mild and self-limiting (meaning they resolve on their own) like Blepharitis and viral conjunctivitis to severe conditions such as Endophthalmitis and Orbital Cellulitis, which may give rise to permanent vision loss and even pose life-threatening complications like brain abscesses. Symptoms can include, depending on severity, location and cause, redness, irritation, photo-sensitivity, and discharge (which could be watery, yellowish, mucopurulent, mucus or a combination). 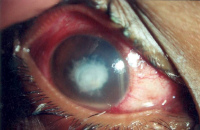
Fungal Eye Infections can be very serious and vision-threatening. Good visual recovery depends on the location of fungal abscess and the extent of damage to the eye before effective anti-fungal medicines have been initiated. Thus, early detection is critical. Infections of the cornea have been categorized into two basic forms: Fungal Infections of the cornea are challenging to treat because: Fungal Infections may arise from a fungal infection in another body part. Many different organisms (including fungi) disseminate via the bloodstream and can directly affect the eye. What are risk factors for Fungal Eye Infections?
Risk factors for Fungal Infections due to filamentous fungi include: Risk factors for Fungal Infections due to Candida Albicans and related fungi include: How are Fungal Eye Infections diagnosed?
Because Fungal Infections can mimic other corneal conditions, you should expect to have your cornea cultured to confirm fungal structures in corneal scrapes or biopsies. This will be especially true if you have an ocular history of trauma with vegetable matter or a collection of the risk factors mentioned above. How are Fungal Eye Infections treated and managed?
The most common approach used to treat infections is using specific anti-fungal drugs, whether topically directly on the eye or by mouth for the body. Other drugs may be used like broad-spectrum antibiotics to combat a secondary Bacterial Infection. In the event that the infection continues to progress in spite of vigorous anti-fungal therapy, surgery may be necessary. Several methods may be used with the goal of removing infectious elements and necrotic (rotting) tissue and other debris, which may hinder complete healing of the infectious location. What are Bacterial Eye Infections?
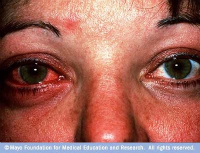
Bacterial Infections can affect the lids, the cornea, or even penetrate the inside structures of the eye. As mentioned above, these internal Bacterial Infections are more vision-threatening, and can even be life-threatening. Bacterial Infections of the cornea have been associated with over wear of soft contact lenses. This type of infection can lead to Corneal Ulcer, which is an open sore on the cornea. The gram-negative rod bacterium called Pseudomonas Aeruginosa is commonly associated with soft contact lens wear. Bacterial Infections of the inside of the eye can be categorized depending on the location of the infection. Preseptal (or periorbital) Cellulitis is the most common infection of the orbital region, typically affecting the tissue of the upper eyelid and surrounding tissues. This type of infection can occur from trauma, which allows Staphylococcus Aureus or Beta-Hemolytic Streptococci to initiate an infection under the skin of the eyelid. Classic symptoms of Preseptal (or periorbital) Cellulitis include low-grade fever, pain and swelling of the affected eyelid. CT scans of the orbit and sinuses are often necessary, especially in children. The antibiotic regimen that your eye doctor chooses for you will be based on the most likely causative organism and whether your immune system is healthy or not. What are Parasitic Eye Infections?
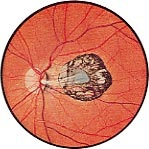
Parasitic Infections are important causes of eye disease worldwide. The geographic location is an important factor in the development of parasitic infections. Other important factors include local sanitation and the presence of a vector for transmission. This class of Infections causes a wide variety of manifestations and can be caused by protozoa, nematodes, cestodes, trematodes and ectoparasites. Toxoplasma Gondii, a protozoan parasite, causes Parasitic Infections which affects millions of persons. Exposure to T. Gondii has been estimated at 30% in the US. Cats seem to be the natural host although raw or undercooked meat (lamb, chicken or beef) are also possible vectors. What are Signs and Symptoms of Toxoplasmosis Infection?Affected children (younger than 12 years) frequently present with: This parasite can be transferred from infected pregnant woman to her fetus and when an infant is born infected, other body complications can occur such as: Teenagers and adults also present with decreased vision along with these other symptoms:
How is Toxoplasmosis Diagnosed?
The diagnosis is based on laboratory testing for detection of antibodies and T. Gondii DNA using Polymerase Chain Reaction (PCR), Antitoxoplasma Antibody Test, Sabin-Feldman Methylene Blue Dye Test, and Compliment Fixation Test How is it Managed?
There are several regimens, each with a different drug combination. The therapy includes specific oral and eye drop combinations. The most common treatment is Bactrim DS (trimethoprim/sulfamethoxazole) one tablet by mouth twice per day for four to six weeks. Uveitis is treated with steroid eye drops and dilating drops. The wide gamut of Eye Infections should stress to you that if you or your loved ones experience any unusual eye symptoms that include, but are not limited to, redness, pain, photophobia (sensitivity to light), decrease in vision, Vitreous Floaters, whiteness of the cornea, double vision or Crossed Eyes, or swelling of your lids, please consult your nearest eye care provider. |




