|
What is a Corneal Ulcer?
Do you have a very red and painful eye? Are you very sensitive to light? Has your vision become blurry? You may have a Corneal Ulcer. 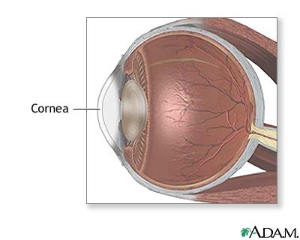
Because the cornea is exposed to the outside, it is susceptible to infections and injury from foreign objects. One foreign object which has often been implicated with ulcers is contact lens use. A Ulcer can have a deep affect on vision whereas one that is located in the periphery of the cornea may not affect vision much. The cornea can become infected by bacteria, viruses, fungi, or a parasite. These infections occur due to some injury to the cornea that makes it vulnerable. What is a Pseudomonas Corneal Ulcer?
Infections of the cornea are the most common, sight-threatening condition associated with contact lens wear. While even daily wear of contact lenses carries an increased risk for infection, sleeping in wear. While even daily wear of contact lenses carries an increased risk for infection, sleeping in contact lenses is the greatest risk factor. Many bacteria have been identified in contact lens related Corneal Ulcer. The gram-negative rod bacterium called Pseudomonas aeruginosa is commonly associated with soft contact lens wear. What does a Corneal Ulcer look like?
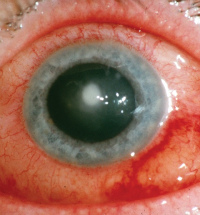
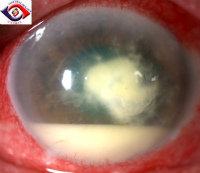
What are other signs of Infection?
Signs and symptoms: How is it managed?
Your eye doctor may perform a culture in order to determine which organism you have become infected with. While awaiting lab results, this will be considered infectious until proven otherwise. Therapy begins with immediate, intensive, aggressive treatment with antibiotics (usually fourth-generation fluoroquinolones or fortified antibiotics in the case of severe ulcers). Dilating drops are valuable to give you comfort and to prevent other complications when you have accompanying Uveitis Steroids can be helpful in quieting the inflammation and thus minimizing subsequent scarring. However, initial treatment should avoid steroids since these drops may worsen an infection. Once the open sore is closed and your eye doctor can see that the infection is subsiding with the prescribed antibiotic (usually after 72 hours of treatment), a steroid may be added to the therapy in order to control persistent inflammation and reduce tissue damage. You will be followed daily at first and your eye doctor will carefully monitor the size of the ulcer and the associated inflammation. Your antibiotic regimen should be reduced depending on your healing progress but should not be tapered below the minimum dosage (usually three to four times a day dosage) in order to prevent the possibility of bacterial resistance. Of course, if the lab results show that a different type of organism is causing the infection, such as fungi, the treatment regimen will be changed accordingly. Make sure you are compliant about your follow-ups to your eye care provider while your infection is resolving. |




