|
What is Strabismus?
Strabismus has often been referred to in layman terms as “Crossed Eyes” or “Wall Eyes”. Strabismus is a condition in which the eyes are not properly aligned with each other. One eye is either constantly or intermittently turned in, out, up, or down. Accompanying the ocular misalignment may be abnormal motility of one or both eyes, Double Vision, Amblyopia, ocular discomfort, or abnormal head posture. In order to view the content, you must install the Adobe Flash Player. Please click here to get started.
Normal depth perception is required for many occupational tasks, as well as many other activities in daily life. Studies comparing binocular (using both eyes) with monocular (using only one eye) performance on a variety of tasks for a group of individuals indicate that Strabismus often leads to inefficient performance on various educational and occupational tasks.
To compound matters, Strabismus may be cosmetically displeasing and produce significant psychological impact on patients. Muscles surrounding the outside of the eyeball (otherwise known as extraocular muscles) are responsible for eye movements. In the case of Strabismus, the muscles are not working in synchrony with each other. A particular muscle may be exerting stronger force than the others and so forcing the eye to move in the direction of its force of action or a muscle may be weaker than the others, allowing the other muscles to dominate the eye movement. 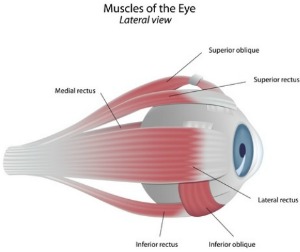
What about Strabismus in Children?
Young children are not routinely screened for Strabismus and even when they are screened, there may be an under-detection of vision problems. Every child should undergo optometric examination by 6 months of age and again at the age of 3 years.Crossed Eyes, otherwise known as Esotropia, is often associated with Hyperopia (or farsightedness), especially in childhood. Everyone needs to focus their eyes like a camera to do near tasks like reading or working on the computer. A person with Hyperopia needs to focus his or her eyes to see clearly at distance, and then focus even more to see clearly at near. When the focusing muscles are used, they cause an associated convergence movement of the extraocular muscles to bring the eyes in toward the nose for near viewing. The problem arises if your child needs to focus at distance and even more so at near viewing, and the associated convergence causes Crossed Eyes. Glasses often can help move the eyes outward by relaxing the need to focus, and thus converge, to see clearly. Some children do outgrow Hyperopia and so the need to wear glasses may decrease with age, but not always. The type of Esotropia associated with Hyperopia is referred to as Accommodative Esotropia, is usually intermittent, and is due to the fluctuating focusing status of the child. In general, Esotropia not associated with Hyperopia is usually constant. When Esotropia develops without any apparent cause in a patient with previously normal binocular vision, it is called acute Esotropia. The sudden Double Vision that usually occurs in this situation may be due to a potentially life-threatening disease and thus requires immediate medical attention.
Some possible causes of acute Esotropia include: The opposite of Esotropia is a turning out of one or both eye(s), known as Exotropia. Any acute Strabismus should warrant immediate medical attention to rule out the conditions listed above. Exotropia may be marked by an eye that turns out the same amount whether looking at distance or near. On the other hand, the eye may turn out more in the distance than when looking at near. This is called Divergence Excess. Perhaps, the eye turns out more at near than when looking in the distance. This is called Convergence Insufficiency (CI). CI, for example, will make it very difficult for you to read for extended periods of time and may result in headaches. These eye turns may be constant or intermittent, and depending on which type, the proper therapy options will be recommended. What about Strabismus in Adults?
If you are an adult with Strabismus, your evaluation and management of the condition may be challenging. The evaluations may be time-consuming, especially if you have a history of prior surgical interventions. Strabismus usually develops in childhood. Acquired forms of Strabismus are more often seen in adults and can be a manifestation of systemic disease such as Thyroid-related orbitopathy, diabetes mellitus, or brain tumor, to name a few. How is Strabismus Diagnosed?
Routine eye exams are the best way to diagnose this disease. If you notice your young child has an eye turn as shown in the pictures above, consulting an eye care provider is your best alternative. Early detection is critical in order to reduce the risk of Amblyopia. Amblyopia is a condition where there is decreased vision in an eye even with the best correction in place. Common reasons for this include a large difference in eyeglass prescription between the eyes or an eye turn. If your child has an eye turn that is constant in one eye and only occurs in that eye, then his or her risk of Amblyopia is greater. The eye doctor will measure your child’s refractive state to check for Hyperopia. Also, the degree of eye turn will be measured. Your child may complain of double vision, and may even close one eye when doing near work. Thus, his or her visual discomfort will also be taken into account in making the diagnosis. The same holds true for you if you are an adult. Your eye doctor will check for the best refraction to correct your vision and dilate your pupils to check for any eye disease. Your symptoms will be considered as well as objective measurements of how much your eye turns. These findings will help the eye doctor decide the best course of action to manage your disease. How is This Managed and Treated?
Depending on the cause, your eye care provider will make a decision for treatment based on several factors such as: If the eye turn is significant and especially if discovered early in life, then surgery can be done to the extraocular muscles in order to align the eye better. The treatment may include any or all of the following options: The therapist measures your progress and asks you about your symptoms and then gives you vision exercises to do at home to strengthen certain muscles. Extraocular Muscle surgery and the use of Botulism Toxin injection has been used as an alternative to conventional extraocular muscle surgery. If the disease occurred acutely, notify your eye doctor immediately as this could be a sign of a serious condition. Treatment of course would be geared to managing the underlying condition causing the disease, and using either a patch or prism to help you deal with the double vision. |





 For example, a student with intermittent Strabismus may avoid reading, resulting in poor academic achievement. Likewise, an employee with intermittent Strabismus may suffer from headaches and fatigue, resulting in reduced productivity.
For example, a student with intermittent Strabismus may avoid reading, resulting in poor academic achievement. Likewise, an employee with intermittent Strabismus may suffer from headaches and fatigue, resulting in reduced productivity.