|
What is Stargardt Macular Dystrophy?
As the name implies, Stargardt Macular Dystrophy , this is a condition that mostly affects the Macula, which is the central portion of the Retina. The Macula is also the most sensitive to light and color. This disease is is the most common juvenile to adolescent-onset macular dystrophy. The estimated prevalence of Stargardt Macular Dystrophy is one in 8,000 to 10,000. It is an inherited disease, typically autosomal (which means the inherited gene is found on any chromosome other than a sex chromosome) recessive, although rare cases of autosomal dominant Stargardt Macular Dystrophy have been reported. In the typical recessive case, a gene from each parent is required for the child to manifest the disease whereas in the rare dominant case, only one gene is required from either parent. Stargardt Macular Dystrophy was first described in 1909 by Dr. Karl Stargardt. In 1963 Dr. Albert Franceschetti first introduced the term Fundus Flavimaculatus, which referred to the presence of ill-defined yellow-white flecks in the deep Retinal layers of the peripheral Retina. Later it was confirmed that Stargardt Macular Dystrophy and Fundus Flavimaculatus both showed disease causing mutations in the ABCA4 gene and some believed it to be the same condition. The mutation in the ABCA4 gene on chromosome 1 affects the rim protein on rod outer segments. Rods are photoreceptors, or cells sensitive to light found both in the Macula and the periphery of the Retina. This mutation ultimately results in the accumulation of lipofuscin in the Retinal Pigment Epithelium (RPE) of the Macula of young individuals. If you have Stargardt Macular Dystrophy, A2E will accumulate in your RPE at an early age, causing degeneration of the macula and loss of vision similar to Age Related Macular Degeneration (ARMD). The compound A2E is stable and not degradable by enzymes, and it comprises the main component of lipofuscin. cula Dystrophy? What are signs and symptoms of Stargardt Macula Dystrophy?
Classic features of the disease include: During eye examination of the Retina, the following findings are possible:
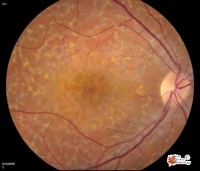
The Macula has a glistening beaten-metal appearance, from RPE atrophy. Some patients who have this disease have Macula changes with no flecks, while others have flecks but no Macula changes. If you have Fundus Flavimaculatus, you may have a somewhat later age of onset and slower progression of the disease, difficulty with adapting to the dark after sunlight exposure, Photophobia,and or Phantom Vision which may be seen in more severe stages of vision loss. This occurs because the brain is attempting to make sense of impaired sensory information. The brain is filling in the blanks so to speak and in so doing may embellish the image making it very real just as it does in our dreams. How is Stargardt Macula Dystrophy diagnosed?
A Stargardt Macula Dystrophy Diagnosis is going to begin, as it does with other eye diseases, with you sharing your symptoms, especially if you are noticing gradual central vision loss. Early in the disease, the Macula may appear normal. This may slow the diagnosis since children may be misdiagnosed with a psychological vision loss. A routine eye examination with dilation may reveal to your eye care provider any or all of the signs discussed above. Diagnosis can be helped by Fluorescein Angiography (FA). FA is a test in which a dye is injected into the arm and the flow of this dye as it enters the eye is studied. The damaged Retina sits above a layer called the choroid which is rich in blood vessels that supply nutrients to the Retina. If you have Stargardt Macular Dystrophy, your FA will show a darkened choroidal flush which is normally bright as the rich vasculature lights up in normal individuals. This is called a “dark” or “silent” choroid. This finding may help in diagnosis although it is not completely diagnostic of the disease. How is Stargardt Macula Dystrophy treated and/or managed?
Unfortunately, there is no medical treatment available at the present for this disease. There are studies being done on animals which offer some hope for future medical treatments for humans. This may one day include the development of a drug that can prevent A2E accumulation and/or decrease lipofuscin build-up. Other animal models have suggested that Ultraviolet protection sunglasses may lessen the formation of lipofuscin. There is no question that the adolescent years are difficult in and of themselves, let alone if you are informed that your vision is failing. This can be devastating news. The best way to cope is to stay informed of the options available to you. As in the case of other visually debilitating diseases, counseling may be helpful. Support groups or interaction between the parents of other Stargardt Macular Dystrophy may be beneficial. Be encouraged that this disease never causes total blindness. Peripheral Vision remains intact. Low Vision care can help you lead very normal lives. You should do well with magnification optical devices. Simple bifocals may be used in the early stages. Later, closed circuit televisions are helpful. Your mobility is usually minimally affected. You may even be able to drive using Bioptic telescopes, but this may be for a limited time. |