|
What is Ocular Hypertension?
Ocular Hypertension refers to high eye pressure readings (known as Intraocular Pressures). If your eye pressure is higher than 21 mm Hg, your eye doctor may become suspicious of Glaucoma and check for other signs of Glaucoma such as loss of peripheral vision or optic nerve damage. 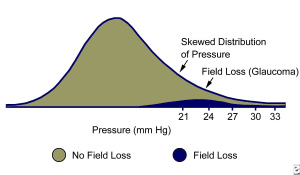
It is not a definitive diagnostic finding. As a matter of fact, you can have high eye pressure and never develop Glaucoma. Because eye pressure alone does not predict Glaucoma, eye specialists have grappled for decades with the decision of whether to use drugs or surgery to lower the pressure in those with Ocular Hypertension in order to prevent glaucomatous damage and when is the best time to do so. One particular study in the ophthalmological community that researched these questions is called the Ocular Hypertension Treatment Study (OHTS). In order to view the content, you must install the Adobe Flash Player. Please click here to get started.
The OHTS had two major goals: The results of the OHTS proved that topical medication does reduce the incidence of glaucoma. After five years of following the patients recruited in the study, the researchers determined that eye drop treatment reduced the development of glaucoma by more than 50 percent. The OHTS researchers also conducted a detailed analysis to determine which patients were at greater risk for developing glaucoma. Predictive factors found in the study were: Based on these factors, the researchers were able to demonstrate that some patients with Ocular Hypertension are at very low risk of developing Glaucoma, as low as 1-2% over five years, whereas other groups are at a much higher risk, as high as 25-35% over five years. Thus, some of these participants might benefit from receiving early treatment while others are at such low risk that it may not be worthwhile to treat them. How Does Your Eye Doctor Differentiate Between Ocular Hypertension and Glaucoma?
Your eye doctor will gather a variety of clinical data about you in assessing your risk of developing Glaucoma if you have Ocular Hypertension. Some of the clinical data will be objective findings such as: Glaucoma is considered the second leading cause of blindness worldwide and sadly, a significant proportion of at-risk patients remain undiagnosed, untreated or undertreated. Why does this occur? Glaucoma has no symptoms. More than likely, you will not feel pain in your eyes from high eye pressure. You won’t be able to notice the subtle progressive vision loss in your peripheral fields with time until it is so obvious that it is too late. Even patients who are diagnosed and being treated may fail to use their eye drops as directed because their vision is good and because they have no symptoms. You can think of Glaucoma as being similar to High Blood Pressure. High Blood Pressure has no symptoms in general. You may get headaches when it is severe, but by and large, you don’t get symptoms. Meanwhile uncontrolled and/or untreated High Blood Pressure can put you at risk for Stroke (even if you are younger), wreak havoc on your kidneys, affect your heart, and eventually kill you. Similarly, Glaucoma that is uncontrolled and/or untreated can put you at risk for Eye Strokes, progressive damage to your Optic Nerves, progressive peripheral Visual Field loss, and eventually blind you. Glaucoma affects the circulation to the Optic Nerve and without oxygen and nutrients, the nerve dies. How can you prevent this? Go to your eye doctor for regular eye exams (at least every one or two years), especially if you have multiple risk factors. Do this even if you don’t need glasses and see very well. Since there is a link between Metabolic disorders like Diabetes and High Blood Pressure, do all you can do to lower your risk of getting these diseases such as keeping your weight down, taking multivitamins, exercising, and avoid smoking. In addition to objective clinical findings, your eye doctor will assess other risk factors in deciding when to treat such as: The more risk factors that you have, the more likely your eye doctor will choose to treat. What Should You Do When You Have Both Cataracts and Ocular Hypertension?
Cataracts are a clouding of your crystalline lens. Cataracts can dramatically lower your quality of life if they are mature enough.The crystalline lens can become cloudy and obstruct your vision. 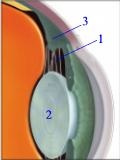
This clouding is more typically age-related, but certain medications or trauma can cause it as well. In diagram, the following structures are represented by the numbers: 1. Zonules 2. Crystalline Lens 3. Ciliary Body When Cataracts are adversely affecting your vision to the point that they are precluding you from participating in normal activities safely (such as driving), then they need to be extracted and a man-made implant inserted in its place. Cataract surgery has evolved into an extremely safe procedure and may even lower intraocular pressure! Thus, if you have Ocular Hypertension and then get diagnosed with Cataracts, don’t hesitate to speak to your eye surgeon about risks and benefits. |




