|
What is CMV Retinitis?
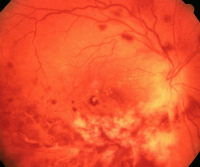
CMV is a well-recognized, vision-threatening, and organ-invasive manifestation of Cytomegalovirus infection in individuals with a decreased ability to fight infection (such as AIDS patients). Cytomegalovirus, a common virus, is a member of the herpes virus family. It infects most people at some time during their lives but rarely causes symptoms. Like other herpes viruses, CMV infection can become dormant for a while and may reactivate at a later time. What causes CMV?
CMV is not highly contagious and is not associated with food, water or animals. However, it can spread from person to person by direct contact. The virus is shed in body fluids such as the urine, saliva, and semen. The critical component in fighting the viral infection is an intact immune system. CMV Retinitis gained attention with the emergence of HIV infection in the early 1980s as it became known as one of the major manifestations of AIDS. CMV Retinitis was first described in patients who received certain types of chemotherapy for cancer treatment as well as those who received immuno suppressive therapy against graft rejection. Although CMV Retinitis is fairly rare for those who have had organ transplants, it has a fairly complex clinical course and severe morbidity (high risk of vision loss) when it does occur in post-transplant patients. So what is the connection between CMV Retinitis and your immune system? The answer lies in the infection-fighting white blood cells, namely those called CD4. CD4 cells are also referred to as T-cells, “helper” cells, or CD4+. When HIV infects humans, the cells it infects most often are CD4 cells, which are an important part of the immune system. The genetic code of the virus then becomes part of the cells and when CD4 cells multiply to fight an infection, they also make more copies of HIV. If you have had HIV for a long time, the number of CD4 cells goes down. This is a sign that your immune system is being weakened. The lower your CD4 cell count, the more likely you will get sick. There are millions of different families of CD4 cells, each designed to fight a specific type of pathogen. When HIV reduces the CD4+ count, some of these families can be totally wiped out and you can lose the ability to fight off the particular germs those families were made to fight. This puts you at risk to develop an infection of that germ. This is referred to as an opportunistic infection, which CMV Retinitis is one. CMV Retinitis develops overtly in 20% of HIV infected individuals within 2 years once the CD4+ counts have fallen below 100/mm3. Maintaining your CD4 count high can reduce HIV complications such as CMV Retinitis and extend your life and vision. How is CMV diagnosed?
CMV is best diagnosed by careful examination of the retina through a dilated pupil. The retinal findings are usually distinctive enough that other diagnostic procedures are rarely needed. See diagram above. There are exceptions of course. Exceptions include unusual cases of CMV or infections with other pathogens for those who are at high risk for CMV Retinitis. These unique situations may require invasive diagnostic testing of ocular fluids or tissues. Even if your doctor makes an educated guess on the diagnosis based on his knowledge and experience of various infections, this can lead to a treatment trial with specific drugs that may help confirm the diagnosis by curing the infection. Lab tests (such as examination of serum or intraocular fluids for host antibodies) and confirmation of an infection of the same type in another part of the body may also be used in diagnosis. One feature to keep in mind with CMV is that the virus is very slowly progressive and so the infection may not cause symptoms for a long time before it manifests itself clinically. This fact will help your eye care provider differentiate CMV Retinitis from other more aggressive herpetic retinitis. Routine eye examinations, especially if you have low CD4 counts, are thus important in early detection. CMV symptoms include blurry vision, floaters or blind spots. How is CMV treated and managed?
Treatment for CMV is two-fold: 1. If you have AIDS, then you need medication for the recovery of immune function. Once your CD4 count is increased to above 100 cells/mm3 (and commonly after at least 3 months), reactivation of CMV is unlikely. The way the immune system is treated is with highly active antiretroviral therapy, otherwise known as HAART. HAART therapy is continued for the remainder of your life. 2. By contrast, the specific treatment for CMV Retinitis is usually required for only a limited amount of time. The agents typically used to treat this condition are: |




